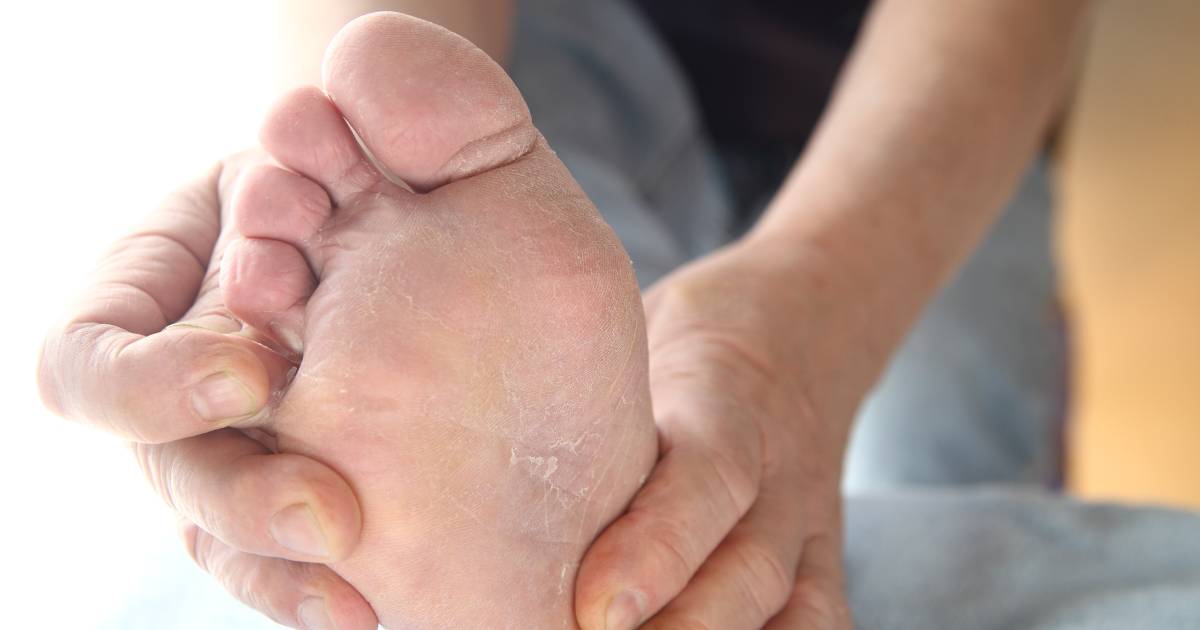
Athlete’s foot (tinea pedis) is the most common type of fungal skin infection and usually presents as a rash on the skin of the foot. There are three main types of athlete’s foot:
| Toe web infection |
|---|
|
| Moccasin infection |
|---|
|
| Vesicular infection |
|---|
|

What Causes Athlete’s Foot?
Athlete’s foot is caused by an overgrowth of tinea, a contagious fungal infection. Fungi grow best in warm, wet places on the body and often thrive in Singapore due to the moist and humid environment.
It is important to note that fungal infections are transmissible between individuals. Factors that can lead to a tinea pedis infection include:
- walking barefoot on moist wet surfaces such as those near swimming pools or in locker rooms
- coming into contact with an infected person
- coming into contact with a contaminated surface
If you have a weakened immune system due to autoimmune diseases, diabetes or other long-term procedures such as chemotherapy, please seek podiatric care promptly if you notice any signs of athlete’s foot. Athlete’s foot is a fungal infection that can spread to other parts of the body if left unaddressed. This can further weaken your immune system and make you more susceptible to other infections.
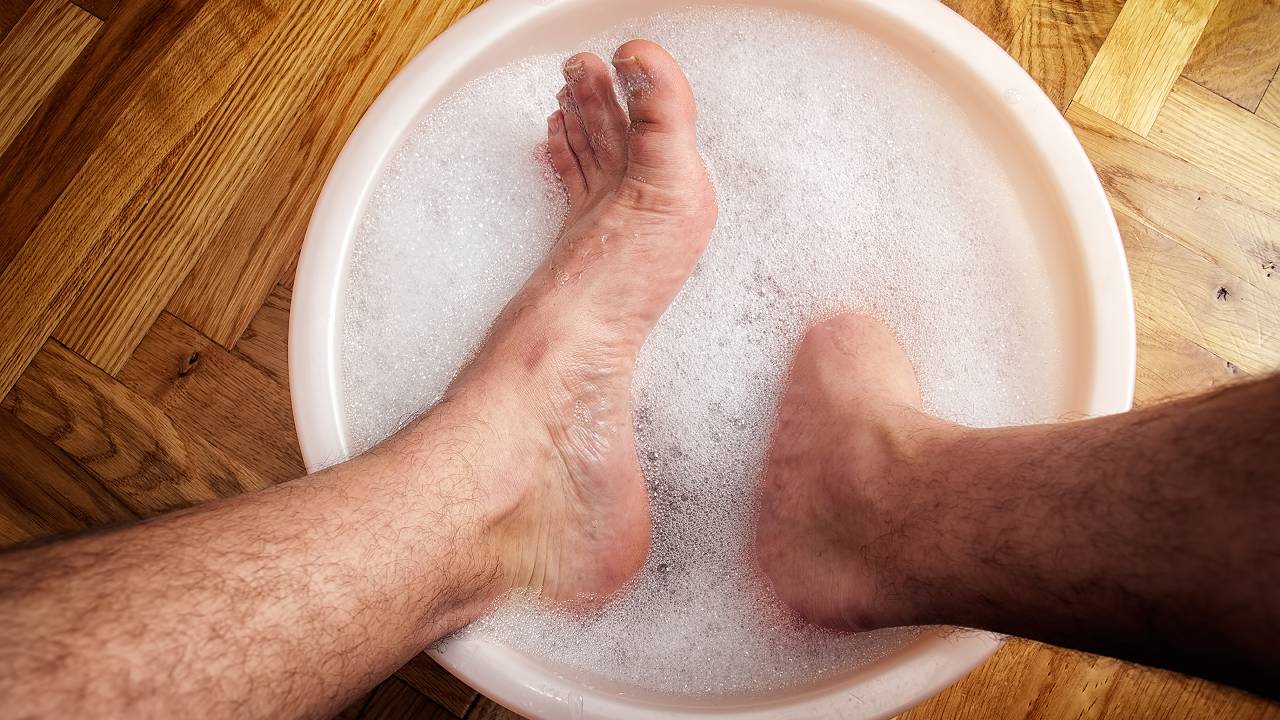
How To Manage Athlete’s Foot?
Home remedies such as talcum powder or vinegar foot soaks may be effective in managing mild cases of athlete’s foot. However, If these remedies do not work, or if the infection worsens, it is important to speak to a foot specialist or podiatrist.
Podiatrists can diagnose and manage a variety of lower limb conditions, including fungal infections like athlete’s foot. To provide the best possible care, podiatrists will conduct a thorough examination of the affected area to confirm the diagnosis, before prescribing the most appropriate solution, which may include topical and oral medication, or antimicrobial therapy. Podiatrist can also provide advice on how to speed up the recovery process and prevent the infection from worsening.