Many believe bunions to be a condition that only occurs in adults but the onset of juvenile bunions can happen in children after the age of 6, or in rare cases, in children as young as a year old.
Bunions are typically characterised as a bony bulge or swelling at the base of the big toe joint. They are not a formation of soft tissue as many assume they are, but are in fact a result of early bone deviation or protrusion.
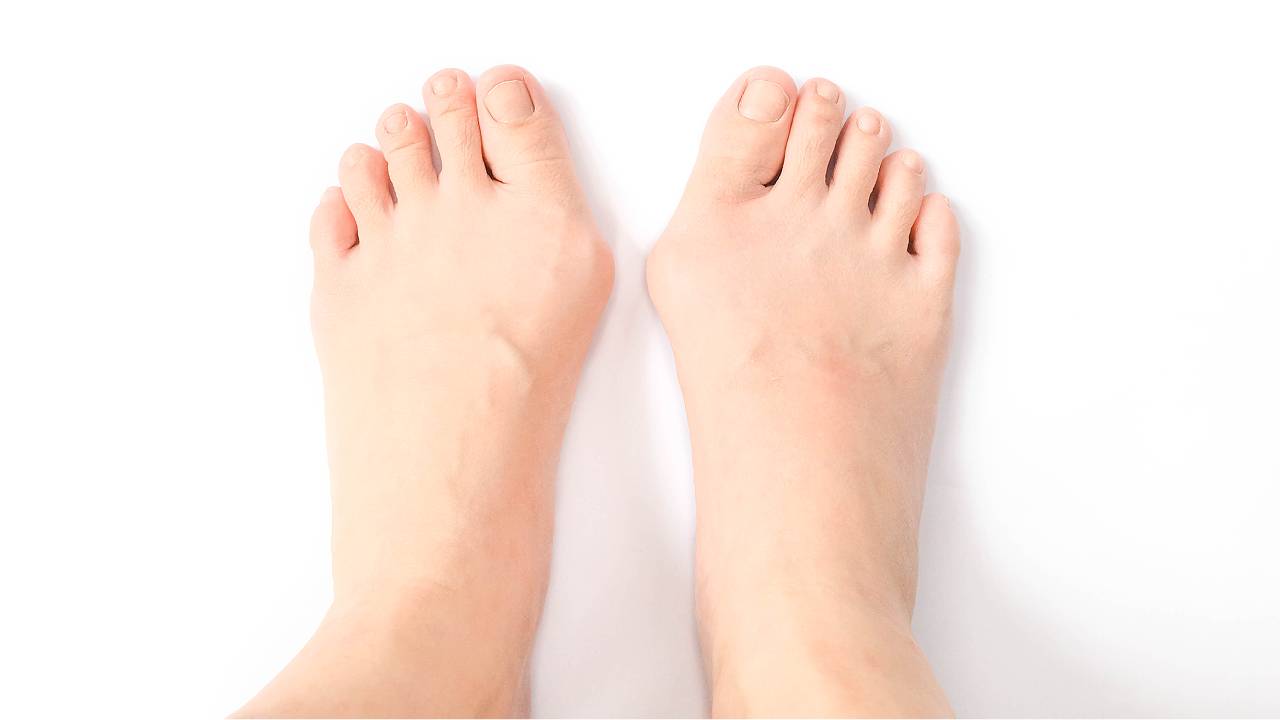
What Causes Bunions In Children?
A child’s bones are especially susceptible to deformative forces during their growth. Juvenile bunions, which can be more severe than adult-acquired bunions, can occur if underlying issues are not rectified. Such underlying issues include the presence of flat feet in young children, which imposes stress upon the ligamentous structures of the feet, leading to postural instability, early joint deformity, and damage.
The causes for bunion development during childhood vary. These factors can include:
- Hereditary Transmission
- Flat Foot
- Hypermobility
- Trauma
- Poor-fitting footwear
- Underlying rheumatological conditions
- Underlying neurological disorders
The main cause of bunions worldwide appears to be related to genetics. It is not uncommon for podiatrists to see a history of bunions across multiple generations in a patient’s family. If you or other members of your family have bunions, you should check your child’s feet regularly for any signs of bunion development.
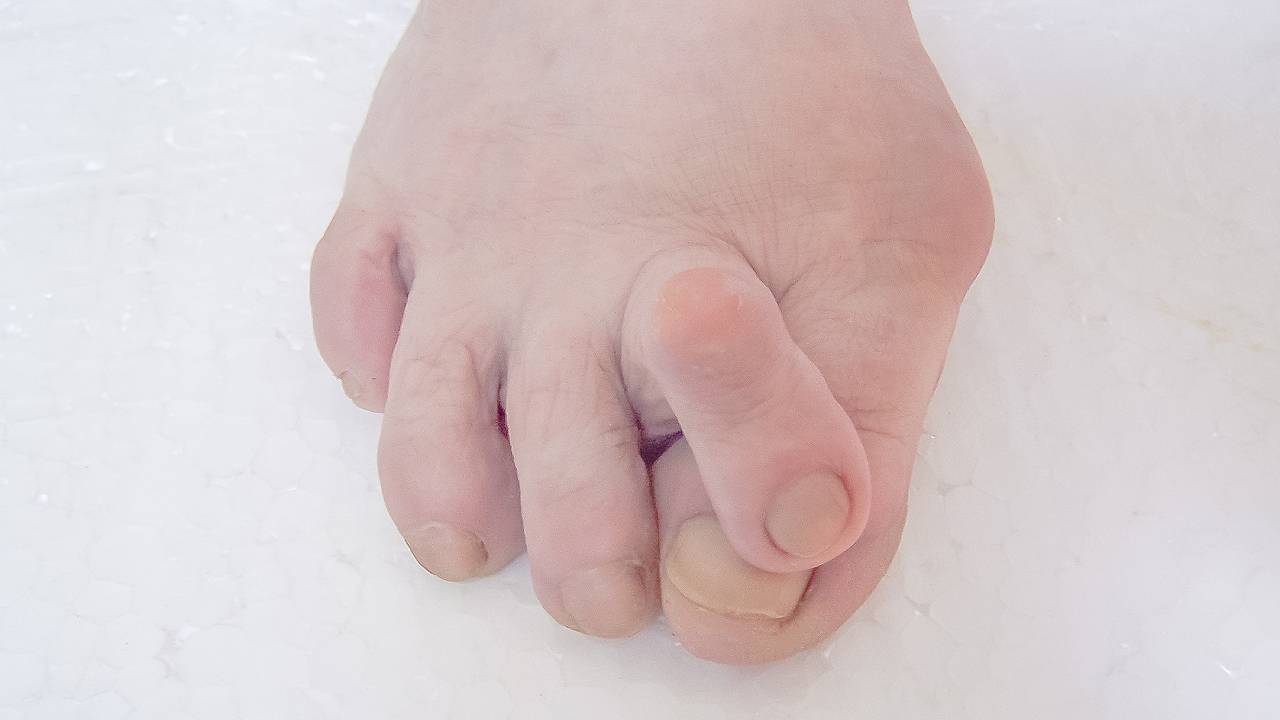
Symptoms Of Juvenile Bunions
Problematic bunions in children will usually cause:
- Soreness at the bunion site
- Irritation from wearing tight shoes
- Discomfort when walking
- Possible instability leading to tripping and falling
- Other pains related to overall foot shape and muscle overuse
Patients with unresolved juvenile bunions will frequently experience:
- Pain in and around the toe, and the development of corns at pressure points
- Redness and swelling at the joint
- Restricted movement of the toe
- Deviation of the big toe towards the second
- Transferring of weight to other parts of the foot to relieve pain
In some cases, patients will feel little or no pain with the only symptoms of bunions being visible bumps on the feet. However, even though there might not be any immediate pain, bunions can worsen and lead to secondary problems higher up in the body such as at the ankles or knees.
What Should I Do If My Child Has Bunions?
Paediatric foot deformities can be subtle but will eventually present with permanent pain if they are neglected. Severe bunions can cause the toes to overlap, subluxate (partially dislocate), or wear out the protective cartilage of the joints. These changes will result in joint pain and reduced mobility, limiting footwear options.
Once a bunion is identified, it is advised that early conservative steps be taken since the growth plates of children have not fused yet and are still malleable. This is to prevent the deformity from worsening into a stage that requires surgical correction.
Parents who suspect bunions in their child should seek prompt consultation with a lower limb specialist. Your podiatrist will perform a thorough physical assessment and diagnostic imaging to determine the severity and cause of the deformity.
Intervention depends on the severity of bunion but can include:
- Recommendations on specific supportive footwear
- Customised orthotic inserts to redistribute weight and relieve pressure on the feet
- Ankle-foot orthotics (AFO) to reduce lower limb malalignment and rotational deformities
- Night splints
- Specific foot exercises and stretches
- Extracorporeal shockwave therapy for symptomatic relief
In Singapore, bunion surgery is a common option for adults, but it is not recommended for children, This is because surgery can disrupt the development of their growth plates.
If surgery is unavoidable due to persistent and significant pain, rigid deformity, or impairment of daily activities, it should only be performed after the growth plates are closed.
After surgery, the use of customised foot orthotics is recommended to correct the primary cause of the bunion, the individual’s foot shape and biomechanics. These orthotics are also used to prevent relapses and preserve the optimal post-surgical alignment.
Frequently Asked Questions
Yes, genetics can play a role in determining your foot type and risk factors for developing bunions. However, footwear choices, activities, and habits of an individual can contribute greatly to the formation of bunions as well.
Yes. Slippers and other unsupportive footwear are not recommended for feet that have yet to reach skeletal maturity as they will alter the biomechanics of the foot. Footwear that is too tight, small, or unsupportive can squash the toes together and cause them to curl or lead to deformities such as flatfoot and clawed toes.
While conservative solution can help to relieve pain and improve the appearance of bunions, it is not guaranteed that bunion deformity can be straighten out completely as each individual is unique. However, customised devices may help to guide the growth of the foot and offload pressure from the bunion. This relieves pain and may lead to further improvement over time.
Many factors can also contribute to the improvement of bunions:
- Age of child at the time of intervention
- Severity of the bunion
- Foot arch and type
- Types of activities participated in
- Type of footwear
There is no ideal age for intervention, but early intervention is key to achieving the best results. Parents may notice a mild bunion formation with a flattened arch shortly after their baby starts walking. Repeated and practiced walking patterns will encourage arch development, and a more pronounced arch profile should be seen when your child is as young as 2 years old.
It is not advisable to take a “wait and see” approach in hopes that the condition will improve on its own. Bunions are joint deformities caused by pressure and imbalance, and they will rarely resolve without conservative intervention.
The effectiveness of intervention for bunions depends on the stage of the condition. Early intervention is key to achieving better outcomes, help to prevent the deformity from becoming more pronounced and help guidance of the foot during growth.
If podiatric intervention is delayed, aesthetics will have to be overlooked in favour offloading the joint, as restoring function and minimising the chances of long-term problems should take priority.
In many paediatric cases, bunions do not present with pain except when wearing narrow footwear. Pain is typically only common once the foot is mature and after years of pressure have been placed upon the joint. As a result, parents have to be mindful and observe their children’s feet as the child may not bring it to their attention due to the lack of pain and discomfort.
Yes. Juvenile bunions are deformities of the foot joints due to tissue imbalance and are not a normal occurrence. Aside from visual identifiers, the presence of early bunions can be detected from associated symptoms such as tightness in new shoes, tiredness, and a reluctance to engage in activities.
Unaddressed juvenile bunions can lead to early joint wear and tear in adulthood. This can lead to pain, difficulty walking and even disability. Therefore, receiving podiatric intervention in the early stages is key to preventing juvenile bunions from becoming more severe.




