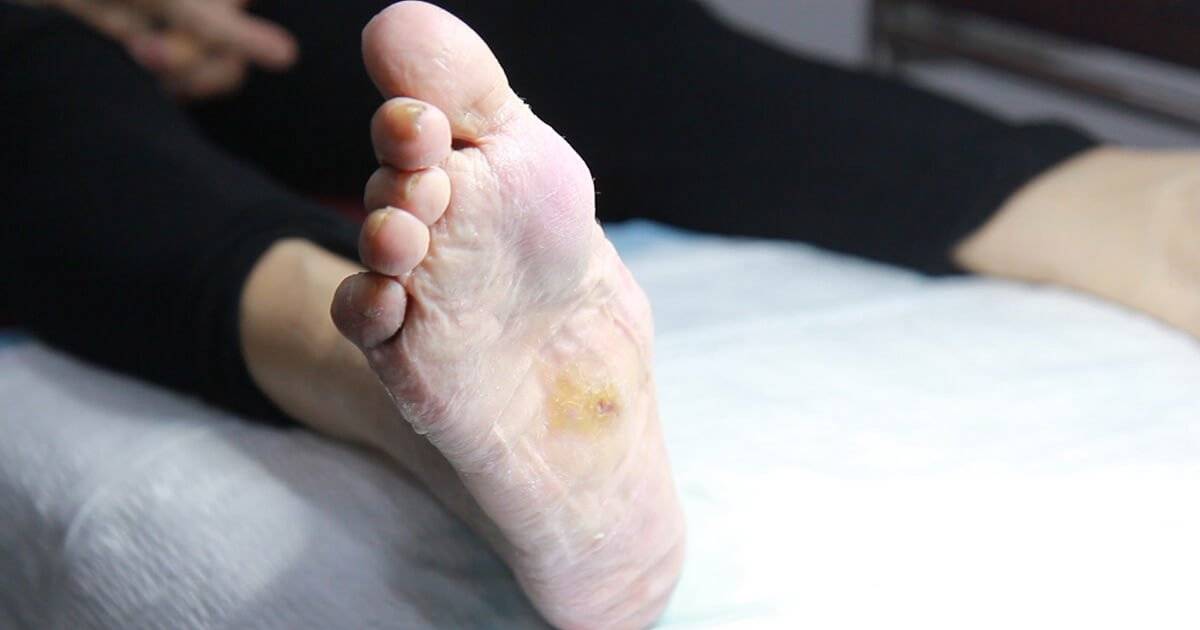
What is Charcot Foot/ Charcot Osteoarthropathy?
Charcot foot, also known as neuropathic osteoarthropathy, is a degenerative complication that can arise due to diabetes. High glucose levels in the body damage the nerves in the lower limbs, causing neuropathy, or numbness and reduced sensitivity.
This lack of sensation then leads to breakdown in the bones, joints, and soft tissues due to the continuous and unintentional pressure on the lower limbs.
Charcot foot occurs in stages:
- Inflammation from acute or chronic trauma leads to osteolysis (breakdown of bone)
- Abnormal vascular reflex increases active bone resorption, making bones weaker
- Spontaneous bone fractures prompt the body to release pro-inflammatory cytokines that promote inflammation, leading to some degree of pain within neuropathic diabetics
- Lack of sensation leads the diabetic patient to continue with normal motion, causing further irreversible damage to the foot
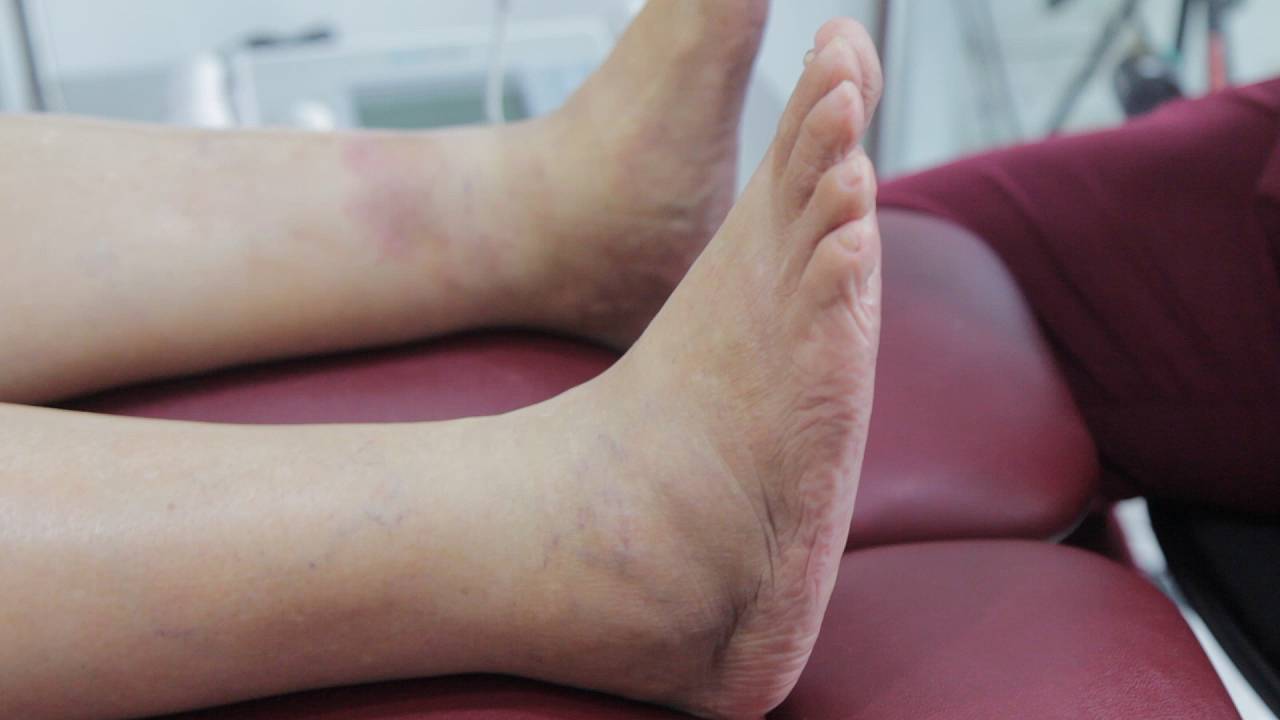
What Does Charcot Foot Look Like?
Charcot foot can result in the destruction of bone, complex fractures, and unrelenting structure deformation of the foot and ankle. The hallmark rocker-bottom foot deformity is a typical late-stage presentation of a diabetic patient with Charcot osteoarthropathy, and can often be mistaken for adult acquired flatfoot disorder (AAFD). Symptoms of Charcot foot can also be mistaken for conditions like cellulitis, deep vein thrombosis, and acute gout.
Symptoms of Charcot foot include:
- Swelling
- Warmth
- Inflammation
- Mild to moderate pain and discomfort
- Temperature difference between two feet
What Happens If Charcot Foot is Left Unaddressed?
Due to the lack of sensation in the foot, charcot foot can lead to open pressure sores, recurrent wounds and ulcers. Bacteria can penetrate deep into the wound, leading to bone infection and a reduction in the function of joints and limbs. In severe cases, it may result in amputation.
Even without the development of foot ulcers, patients with Charcot foot will experience a loss of mobility and an increased risk for falls due to the dysfunctional shape of the foot.
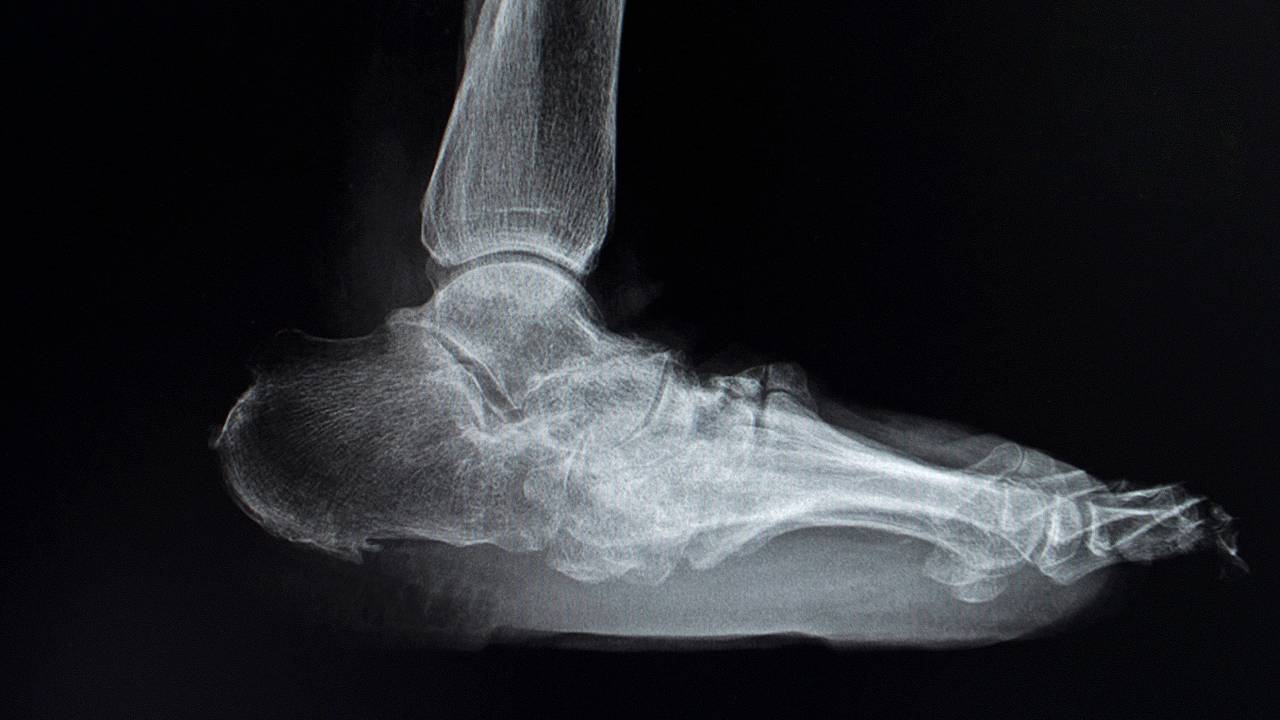
How Can a Podiatrist Help With Charcot Foot?
Podiatrists are trained to recognise the subtle symptoms of a foot undergoing destructive Charcot changes. They will conduct a thorough physical examination and diagnostic imaging to obtain an accurate diagnosis and intervention plan.
Solutions will be customised to the severity of your foot deformity. Some common solutions include:
- Stabilisation of the foot deformity using removable or fixed casts
- Use of advanced non-invasive modalities such as extracorporeal shockwave therapy to reduce pain, swelling, and other symptoms
- Offloading and redistribution of abnormal pressure across the feet through the use of specialised orthotic devices
- Management of open wounds
- Prompt referral for surgical intervention if required
If you think you may have Charcot foot, it is important to see a foot specialist or podiatrist as soon as possible. Early diagnosis and intervention can help to prevent the progression of the condition and reduce the risk of complications.