Posterior Tibial Tendon Dysfunction (PTTD) is a progressive condition that affects the foot and ankle, and is a leading cause of Adult Acquired Flatfoot Deformity (AAFD).
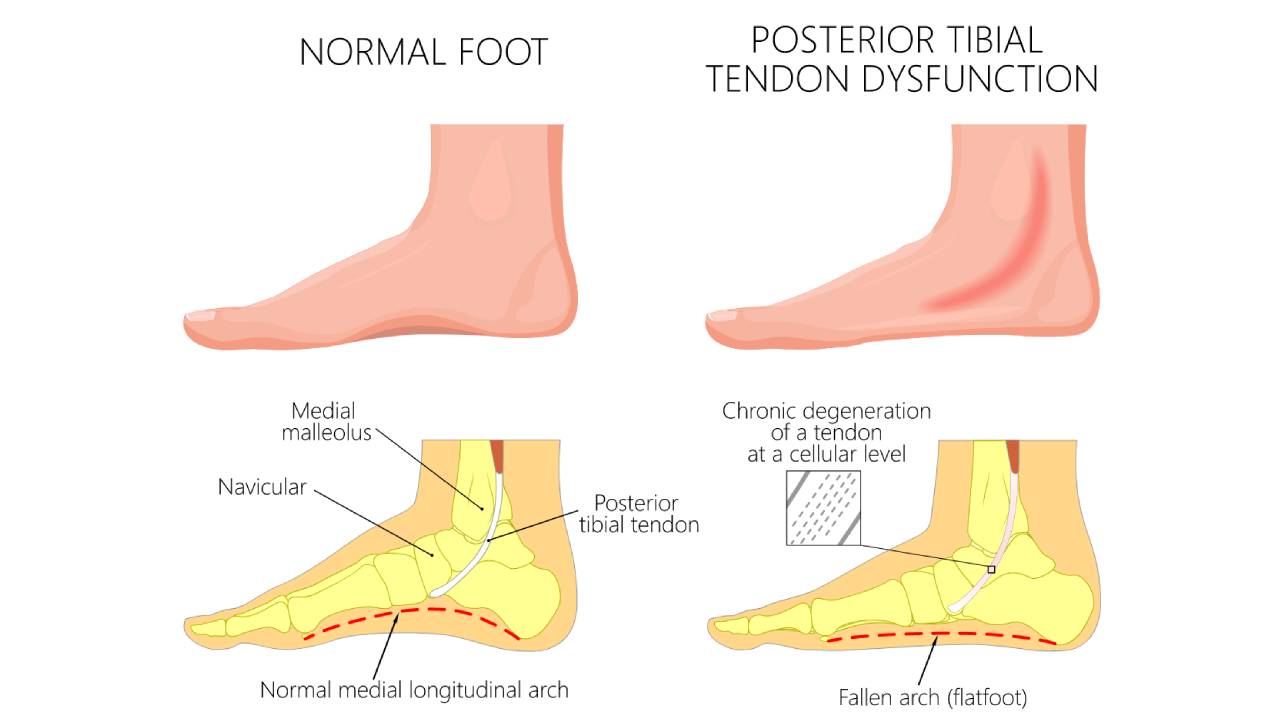
The Posterior Tibial tendon is connected to the Tibialis Posterior muscle. This muscle is located deep in the posterior compartment of the lower leg and is responsible for raising the arch and supporting the foot and ankle during motion. The weakening of this tendon and the failure of ligaments around the foot and ankle is what leads to the collapse of the medial arch and an eventual flat foot deformity.
The majority of PTTD cases arise from repetitive strain to the Tibialis Posterior tendon. Although in some situations, an acute injury may also cause the tendon to tear, resulting in pain and inflammation.
Previously recognised as a common problem afflicting the elderly, PTTD has now become a more apparent issue amongst youths who are overweight, inactive, wear improper footwear such as slippers, or engage in high-impact sports.
Some risk factors of PTTD include:
- Pre-existing flat foot
- Hypermobility
- Being 40 years or older
- Obesity
- Diabetes
- Hypertension
- High impact sports
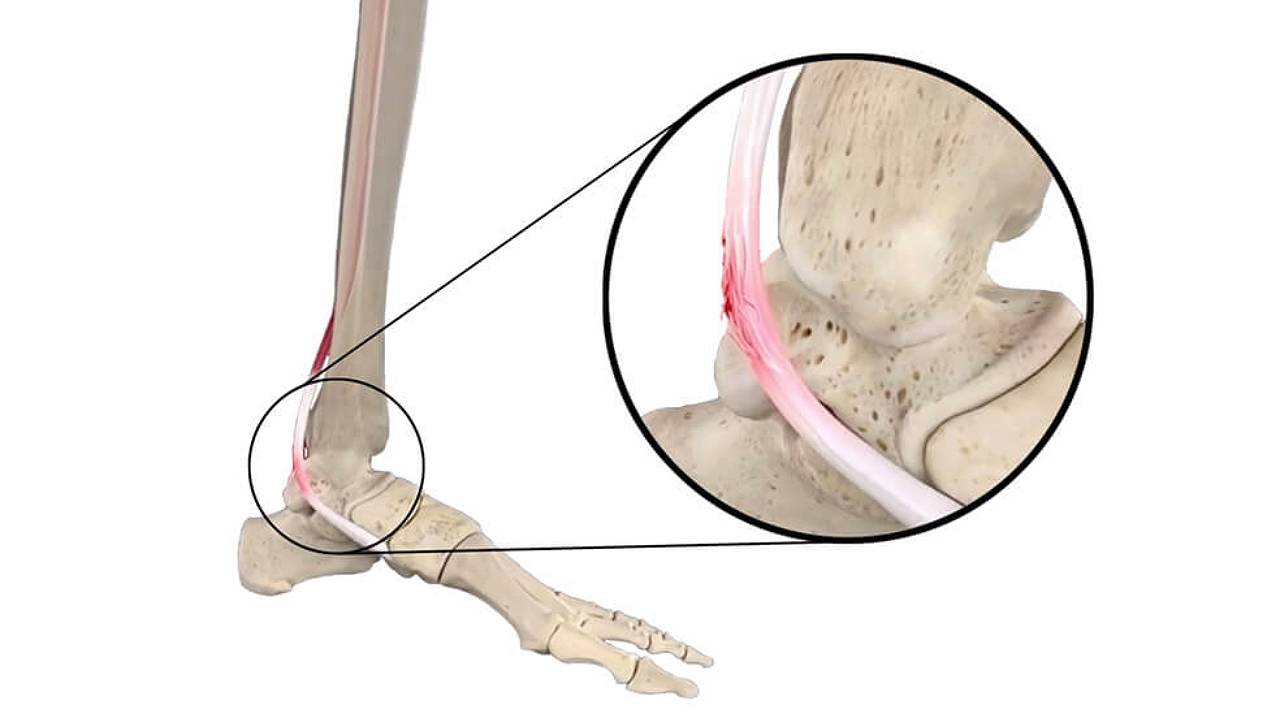
Symptoms of Posterior Tibial Tendon Dysfunction (PTTD):
- Pain presents on the inside of the foot and ankle
- Swelling may or may not be present
- Increased pain and weakness in the foot during physical activities such as walking and running
- A gradual flattening of the affected foot
- Pain in the ankle due to joint impingement from the progressive collapsing foot deformity
- Tingling and numbness due to nerve irritation on the medial aspect of the foot as the foot collapses
How is Posterior Tibial Tendon Dysfunction (PTTD) Diagnosed?
Your podiatrist will assess your foot shape and range of motion to determine the severity and stage of the injury. They may also order imaging tests, such as ultrasound, to confirm the diagnosis. Once the cause of your injury is known, your podiatrist will create an appropriate plan tailored to your individual needs.
How is Posterior Tibial Tendon Dysfunction (PTTD) Managed?

While home remedies such as compression with an elastic wrap or bandage can help reduce swelling. This is not a long term solution. Compression alone is unlikely to resolve the underlying condition, It should only be used as a temporary measure to relief symptoms, before podiatric management is sought.
A podiatrist can include a range of non-invasive options, such as offloading of the affected area and advanced modalities like focal shockwave therapy to stimulate healing and reduce pain.
Custom foot orthotics can be used to offload the injury and prevent flat foot deformity from worsening. Orthotics can also reduce pressure placed upon the tibialis posterior tendon. In severe PTTD or upon visible change to the shape of the foot and ankle, an ankle-foot orthotic (AFO) may be required for adequate support and stability.
PTTD must be managed promptly, If delayed or if non-invasive methods fail to improve symptoms, surgery may be necessary. Do speak to your podiatrist for more information.




