What Types of Heel Pain Are There?
While the most common cause of heel pain in Singapore is repetitive musculoskeletal injury, other more uncommon serious conditions that mimic the pain also exist. It is advisable to see a podiatrist for an accurate diagnosis.
Two terms are commonly used to describe heel pain – plantar fasciitis and heel spur syndrome. For the most part, they are two different names for the same condition, but there are some differences that can impact what we can do for the patient.

Plantar Fasciitis
This describes a recent-onset bout of inflammation at the plantar fascia, which is a thick connective tissue band stretching across the bottom of the foot. The plantar fascia spreads out under the ball of the foot on one end and inserts under the heel bone on the other end.
Recent-onset heel pain describes pain or discomfort lasting fewer than 6-8 weeks. During this period, it is easier to manage the condition because the aim is to focus on resolving the inflammatory process.
In Singapore, many people do not actually have “plantar fasciitis” by the time they get around to visiting a foot specialist; instead, they have something much worse. At this point, the plantar fascia injury has already become chronic, and the initial inflammatory phase is already over. In more serious cases, a plantar fascia tear may even have occurred. Podiatric intervention that focus on improving acute inflammation will have then become less effective or even ineffective for chronic heel pain.
Heel Spur
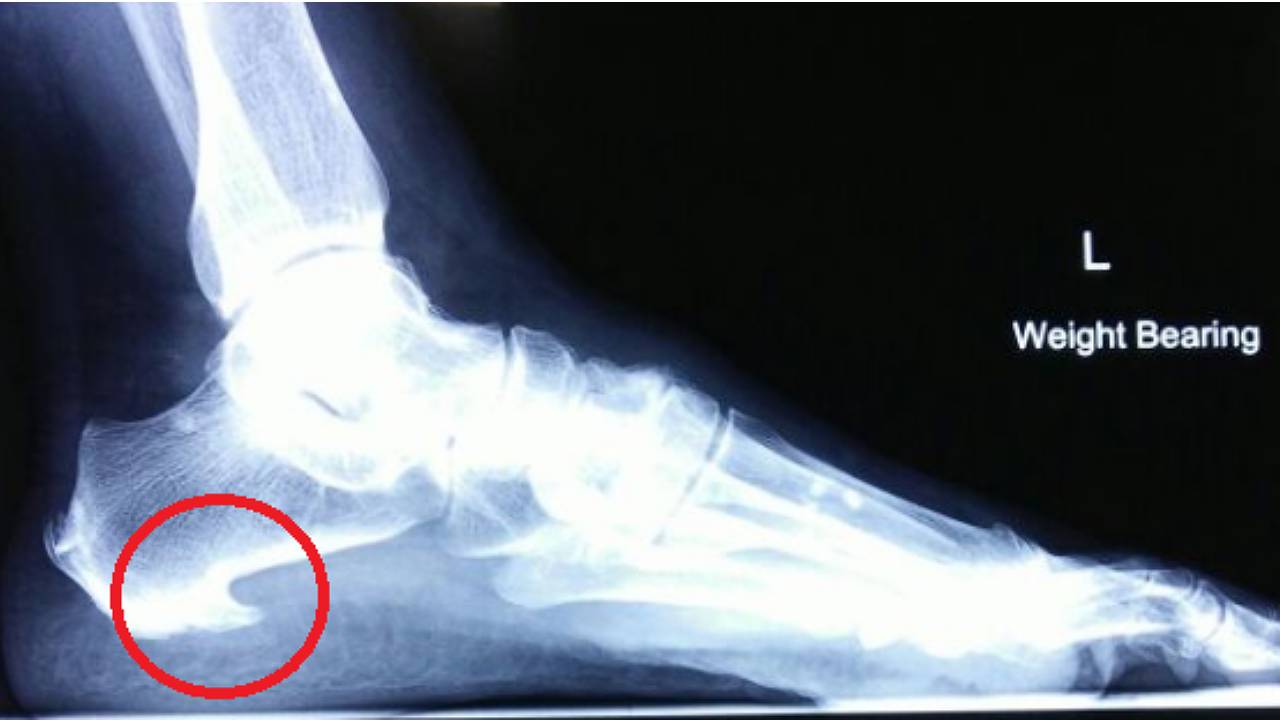
As mentioned previously, many instances of “plantar fasciitis” do not actually involve an inflammatory process. Instead, the plantar fascia is weakened due to chronic collagen degeneration and tissue death. On foot X-rays, those with chronic heel pain may have a calcaneal spur (heel spur). Hence, the name “heel spur syndrome”.
Some chronic cases of plantar fasciopathy do progress to developing calcifications within the plantar fascia itself. However, calcaneal spurs do not necessarily cause heel pain – people without heel pain may also have spurs on X-rays. The “bone spur” is simply the reactive calcification of a plantar fascia undergoing chronic stress. The pathology and pain still stem from the plantar fascia.
The existence of a heel spur suggests that the “plantar fasciitis” has been present for a long time. However, it is not necessary to surgically remove the heel spur to address the chronic heel pain. Instead, conservative options are available for patients who prefer to avoid surgery.
Will it affect my walking in the long term?
We have seen patients who have lived with severe heel pain for years. In most cases, they have altered the way they walk in order to accommodate the pain. This may involve tip-toeing in the morning until the pain wears off or choosing a more sedentary lifestyle. Not only does this lead to a decline in fitness levels, it also encourages the development and progression of other conditions. With the right diagnosis and management, heel pain and other associated conditions can be minimised. Left unaddressed, heel pain can significantly impair your walking and everyday life.
Can I just wait for the pain to subside?
In some cases, rest and home remedies are adequate for the heel pain to subside. However, this does not address the root cause of the pain. Many patients describe having on-and-off heel pain for years that gradually worsens with each episode. The heel pain can always return, and each time it will become more difficult to manage.
Our podiatry clinic focuses on conservative solutions. This approach may include the use of the latest technology and orthotic insoles which are customised specifically to your foot type and your plantar fasciitis (heel pain) condition.
See a podiatrist for a proper diagnosis of the type of heel pain and suitable non-surgical options.
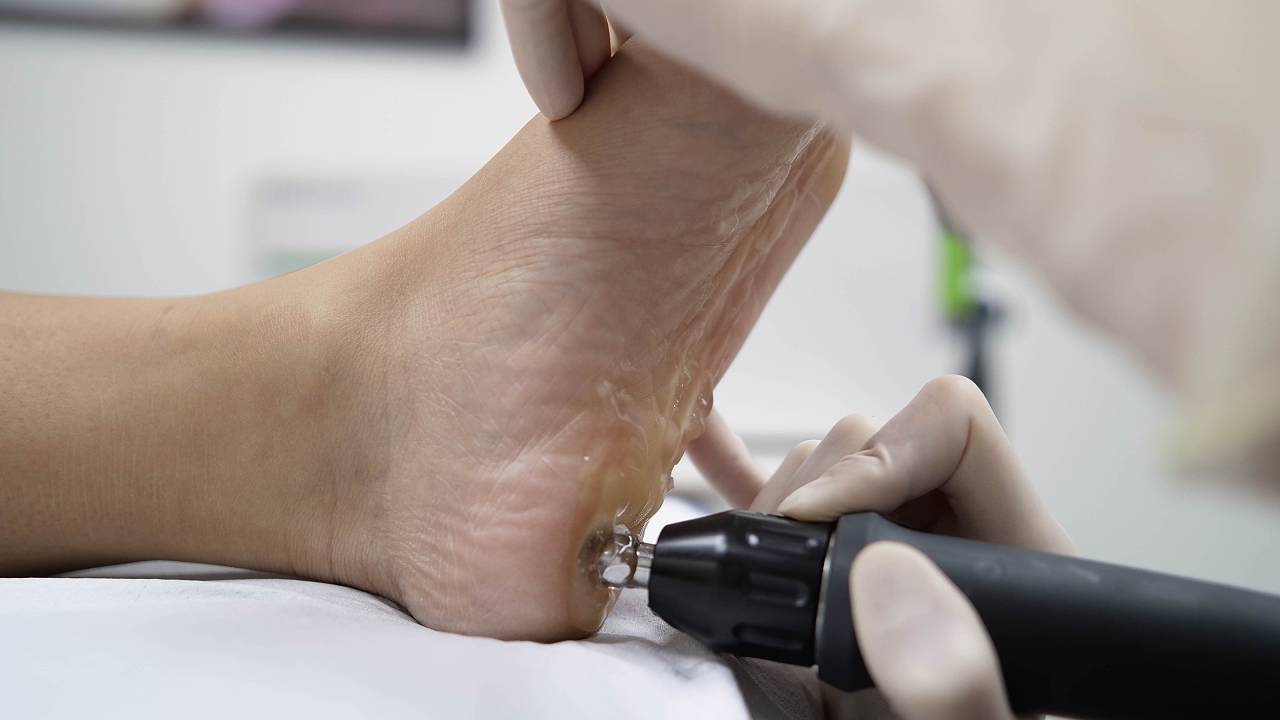
Non-surgical Options for Heel Pain
There are a variety of conservative solutions available, including the use of foot orthotics (shoe insoles), shockwave, EMTT, sports taping, and focused stretching exercises. With the right care and patient adherence, most patients will see significant improvements.
Surgery may be advised if the condition is severe and resistant to conservative solutions. Our podiatrists collaborate with skilled orthopaedic surgeons specialised in foot and ankle procedures. They frequently handle post-operative rehabilitation for lower limb surgeries, including wound care, foot orthotics, and orthopaedic footwear.
Frequently Asked Questions
Heel Pain is a feeling of discomfort or pain in or around the back of the foot. There are many possible causes for heel pain, but some of the most common causes are plantar fasciitis, stress fractures, and tendonitis.
Heel pain can be caused by a variety of factors, including injuries to the foot. These injuries are typically divided into three main categories – Acute, Overuse, and Chronic. Acute injuries are those that are caused by a single traumatic event such as sprains, falls or fractures. Overuse injuries share some similarities with chronic injuries, and are caused by repeated actions that affect a particular group of soft tissues, such as muscles and joints. If left unaddressed, overuse injuries can often become chronic, meaning they last for more than three months and may not heal on their own.
As there are numerous conditions responsible for heel pain, the symptoms also vary widely. Some of the symptoms include swelling or stiffness around the back or underside of the heel, discolouration (typically red), warm skin, limited or painful movement, or discomfort when pressure is applied around the heel.
Plantar fasciitis, which involves an injury to the plantar fascia, is one of the most common causes for heel pain. The plantar fascia is the band of tissue that connects the front of your foot to the heel. It is responsible for supporting the arch of your foot and much of the weight of your body when you are on your feet. As the plantar fascia acts as a shock absorber during movement, they are frequently injured over time. Plantar fasciitis may also be caused by factors such as having a flat or high arched foot, excessive exercise and being overweight.
While heel pain may subside after some rest, the underlying issues that cause it typically persist until it’s resolved. Aggravating factors, such as exercise or being on your feet for long periods of time, can easily trigger the injury once more. Over time, these injuries can result in permanent damage to the plantar fascia, such as a rupture which can only be resolved through surgery.
Heel pain management can be divided into two main approaches: pain relief and addressing the underlying cause. Pain relief can be achieved through a variety of methods including: Analgesics, rest, shockwave therapy, physical therapy and other therapeutic modalities. The second approach is addressing the underlying cause of heel pain. It involves a variety of solutions, depending on specific cause to find out if orthotics or surgery is needed. Therefore, it is critical to seek help as soon as possible to prevent the pain from becoming worse.




